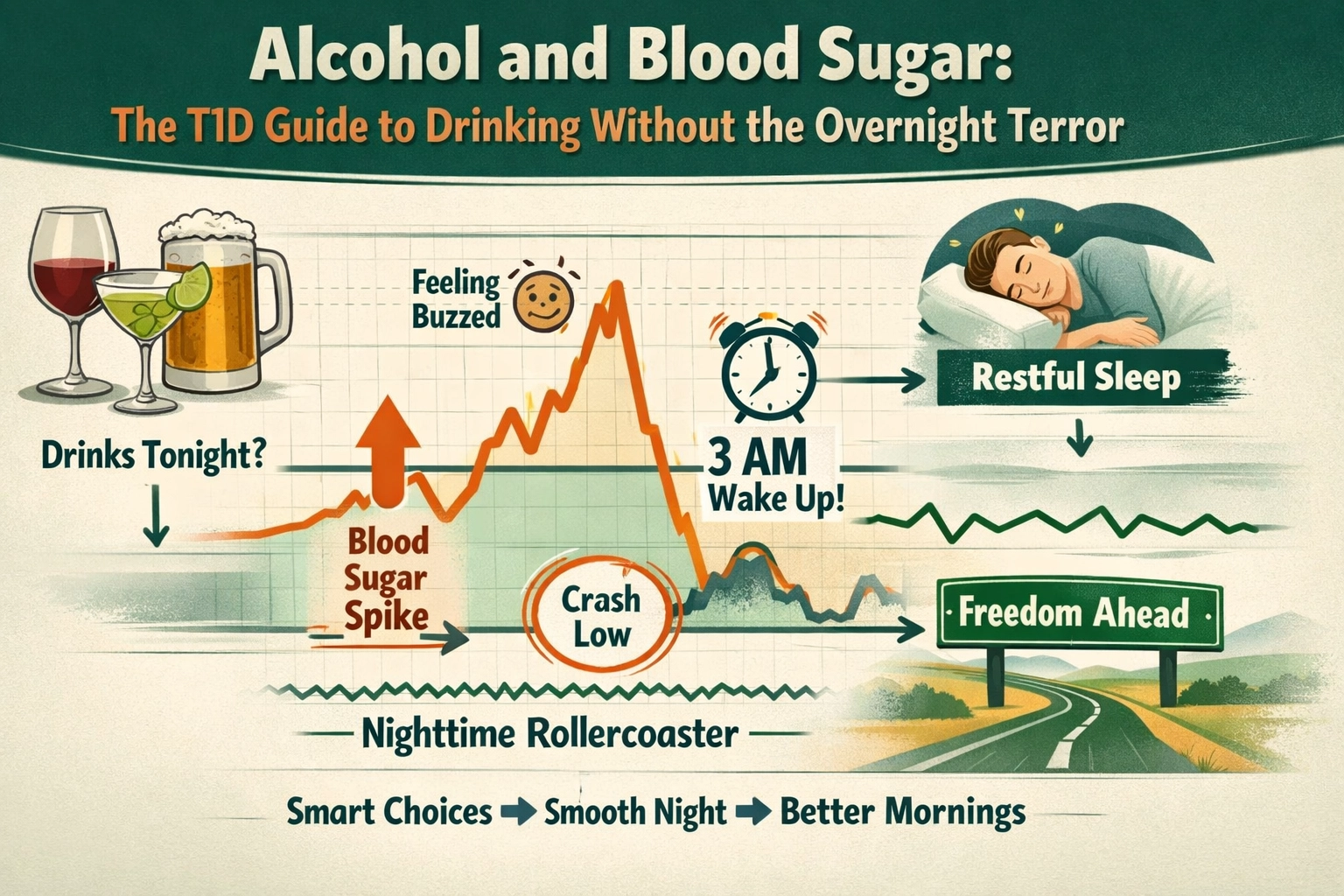
Alcohol lowers blood sugar by temporarily blocking your liver from releasing glucose into your bloodstream. While sugary mixers or heavy beers might cause an initial spike, the primary risk for Type 1 Diabetes (T1D) is delayed, severe hypoglycemia that occurs 4 to 12 hours after your last drink. To drink safely with T1D, you must account for this "liver lockout," prioritize eating while you drink, and adjust your overnight insulin targets to prevent the dreaded 3 AM low.
Let’s be real: living with T1D is a full-time job we never applied for. Most of the time, we just want to be "normal." We want to go to the bar with friends, grab a craft beer at the game, or share a bottle of wine on a date without it feeling like a high-stakes science experiment.
But then the anxiety kicks in. You’re staring at the cocktail menu thinking about the carb count in a margarita, while simultaneously worrying if that same drink will tank your BG while you’re asleep. It’s a total "WTF" moment. You feel like you have to choose between having a social life and staying safe.
We’ve all been there, sitting at a table, checking our CGM every five minutes, trying to do "drunk math" to figure out if we should bolus for the fries or leave the sugar alone to buffer the alcohol. It’s exhausting. It’s chaos. But it doesn't have to be guesswork.
To understand why alcohol is so sneaky, we have to look at the liver. Think of your liver as the body’s ultimate multi-tasker. Usually, it’s responsible for dozens of jobs, but its most important one for us is gluconeogenesis. That’s a fancy word for "releasing backup sugar."
When your blood sugar starts to drop, your liver normally senses it and dumps a steady stream of glucose into your system to keep you stable. It’s your internal safety net.
However, alcohol is a toxin. The moment it hits your system, your liver stops everything else to process it. It’s like a bouncer at a club who stops checking IDs because there’s a fire in the kitchen. The liver is so "busy" detoxifying the alcohol that it completely ignores its job of releasing glucose.

This "liver lockout" means your safety net is gone. If you have active insulin in your system (the "IOB") and your blood sugar starts to dip, your liver isn't going to save you. This is why the risk of a severe low is so much higher when you’re drinking, especially on an empty stomach.
Not all alcohol is created equal in the eyes of a T1D. We usually see a two-stage effect: the Spike and the Dive.
This is where the chaos happens. You bolus for the margarita at 9 PM, but by 1 AM, you’re crashing because the liver can't buffer the drop.
The most dangerous part of drinking with T1D isn't the bar, it’s the bed.
Delayed hypoglycemia is a real threat. Research shows that alcohol can impair your liver’s glucose production for up to 24 hours. Most of us see the biggest risk 4 to 8 hours after our last drink.
When you’re asleep, you’re less likely to feel the physical symptoms of a low. To make matters worse, being "tipsy" feels a lot like being "low." Shaky? Sweaty? Disoriented? It’s hard to tell if it’s the gin or the 55 mg/dL.
If you’ve had a few drinks, your body’s natural "counter-regulatory" response is also dampened. You won’t wake up as easily. This is why we call it the overnight terror, it’s the window where we are most vulnerable and least aware.
We aren't here to tell you not to drink. We’re here to help you do it without the 3 AM ER visit. Control isn't about restriction; it's about preparation.
Every body reacts to alcohol differently. Some of us find that red wine makes us stable, while others find that a single beer causes a 24-hour rollercoaster.
The only way to move from frustration to empowerment is to see the patterns. This is where Subseven comes in. We built it because the standard dosing math (Carbs + Insulin) fails when you add variables like alcohol, stress, or a bad night’s sleep.
When you log your drinks and see how your body responds the next morning, you stop guessing. You start to see: "Okay, every time I have two IPAs, I drop 40 points at 4 AM." Once you know that, you can adjust your strategy. You take the "terror" out of the overnight and replace it with a plan.
T1D is complicated, but it shouldn't stop you from living. You’ve got the tools and now you’ve got the knowledge. Be safe, be smart, and let the data handle the stress.
Does alcohol lower blood sugar immediately?
Usually, no. If the drink contains carbs (like beer or juice), your blood sugar will likely rise first. The glucose-lowering effect of the alcohol itself typically kicks in a few hours later when the liver is busy processing it.
Can I use Glucagon if I have a severe low after drinking?
Glucagon may not work as effectively (or at all) when you have alcohol in your system. Glucagon works by telling your liver to release stored glucose. If your liver is busy processing alcohol, it won't "listen" to the Glucagon. This is why preventative safety is so much more important when drinking.
Is it safer to drink beer or spirits with T1D?
Spirits (vodka, gin, tequila) with sugar-free mixers are "cleaner" because they don't cause an initial spike, but they carry a higher risk of a sudden drop. Beer causes a spike then a drop. "Safe" is subjective, but spirits with a snack are often easier to manage than sugary cocktails.
How long does alcohol affect my insulin sensitivity?
Alcohol can affect your blood sugar and insulin sensitivity for up to 24 hours. You might find you need less insulin for your breakfast or lunch the day after a night out.
What should I do if I’m "low" and "drunk" at the same time?
Always treat the low first with fast-acting glucose (tabs, juice, regular soda). Do not bolus for the "drunk munchies." If you are confused, ask for help immediately.
Should I tell my friends I have T1D before we go out?
Yes. Severe hypoglycemia can look exactly like heavy intoxication (slurred speech, stumbling). Your friends need to know that if you seem "too drunk," it might actually be a medical emergency.
About the Author: Chris Putsch is the CEO of Subseven and has lived with Type 1 Diabetes for years. He’s dedicated to building tools that help T1Ds manage the "hidden variables" of life: like a night out with friends( without the constant mental load.)