
BLUF: Why does exercise affect T1D blood sugar differently every time? It comes down to the "type" of stress you put on your body. Aerobic exercise (like jogging) acts like a vacuum, sucking glucose out of your blood, while anaerobic exercise (like heavy lifting) triggers a "fight-or-flight" response that tells your liver to dump sugar for energy. When you add hidden variables like sleep, stress, and active insulin, the math changes daily. Managing it isn't about a perfect formula; it’s about recognizing your body’s unique patterns.
You did everything "right."
You checked your Dexcom. You had a small snack. You reduced your basal rate thirty minutes before hitting the pavement. You ran the exact same 3-mile loop you ran last Tuesday.
Last Tuesday, you ended the run at a perfect 110 mg/dL. Today? You’re staring at 245 with a diagonal up arrow, and you feel like garbage.
WTF, right?
This is the central paradox of Type 1 Diabetes. Exercise is the "gold standard" for health, yet for us, it often feels like a game of Russian Roulette where the prize is either a terrifying 3 AM low or a stubborn, high-glucose headache.
It’s infuriating. It’s exhausting. And honestly, it’s enough to make you want to stay on the couch. But here’s the thing: your body isn't actually being random. It’s just processing a dozen variables at once that your doctor probably didn't have time to explain in your 15-minute checkup.
If T1D was just about "Carbs in vs. Insulin out," we’d all have 5.0 A1Cs and a lot more free time. But the body isn't a calculator; it’s a biological machine that responds to stress, intensity, and timing.
The biggest reason the same workout produces different results is the metabolic context of your body at that exact moment.
Think of your muscles like a sponge. Usually, that sponge is a bit stiff. It needs insulin (the key) to open up and soak up the glucose (the water) from your blood. When you exercise, those sponges soften up. They can suddenly soak up glucose much more efficiently, sometimes even without much insulin at all.
But the "rate" at which they soak up that sugar depends on what else is happening in the background. Were you stressed at work? Did you sleep four hours? Do you have "stacking" insulin from a late lunch?
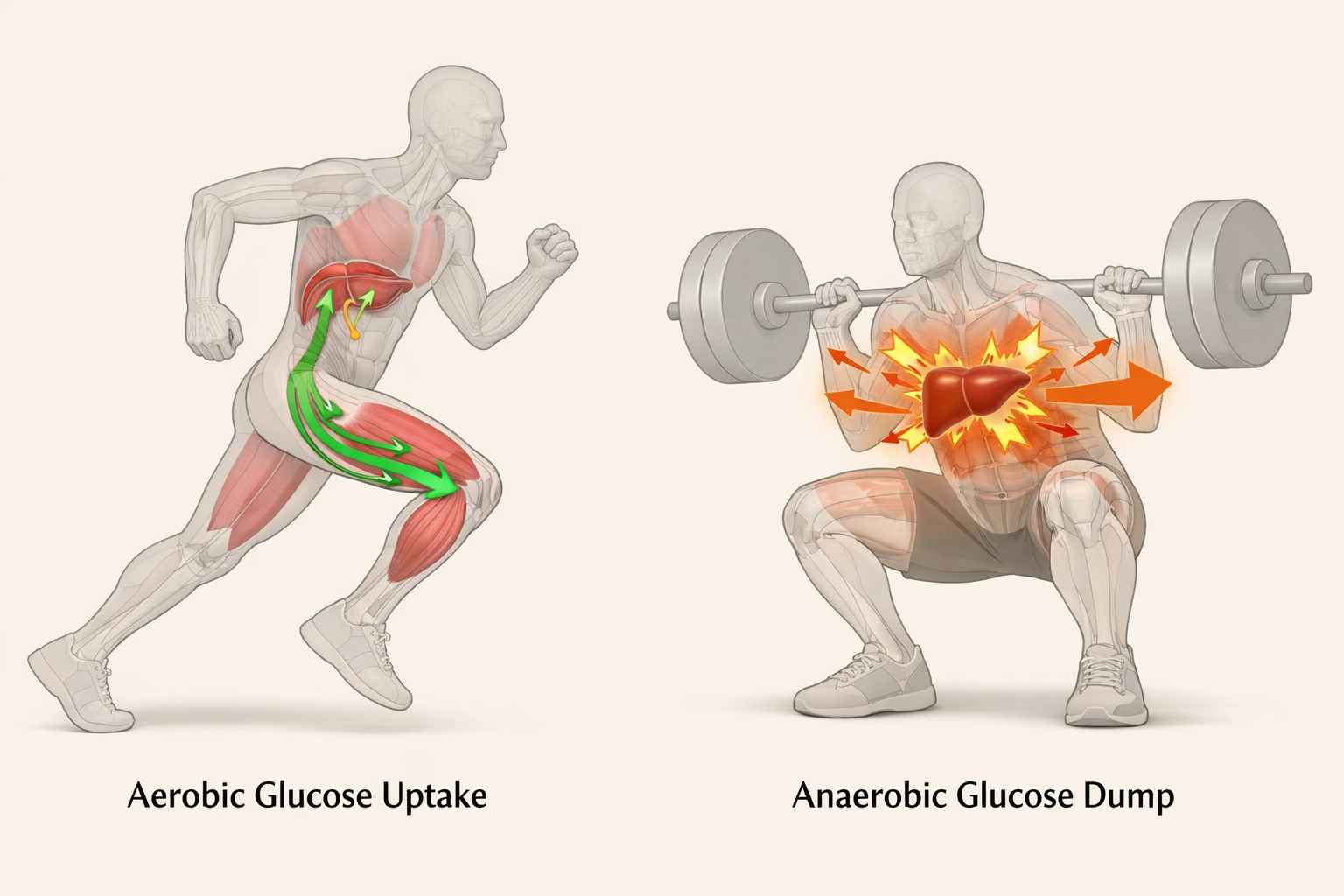
To stop the guessing game, we have to look at the "mode" of exercise. This is the "Engineer" part of the equation. Your body has two main ways of burning fuel, and they have opposite effects on your blood sugar.
Activities like jogging, swimming, or a long walk are "aerobic." Your heart rate stays steady, and your body uses oxygen to fuel your muscles.
Activities like sprinting, heavy weightlifting, or a high-intensity CrossFit WOD are "anaerobic." These are short, explosive bursts of energy.
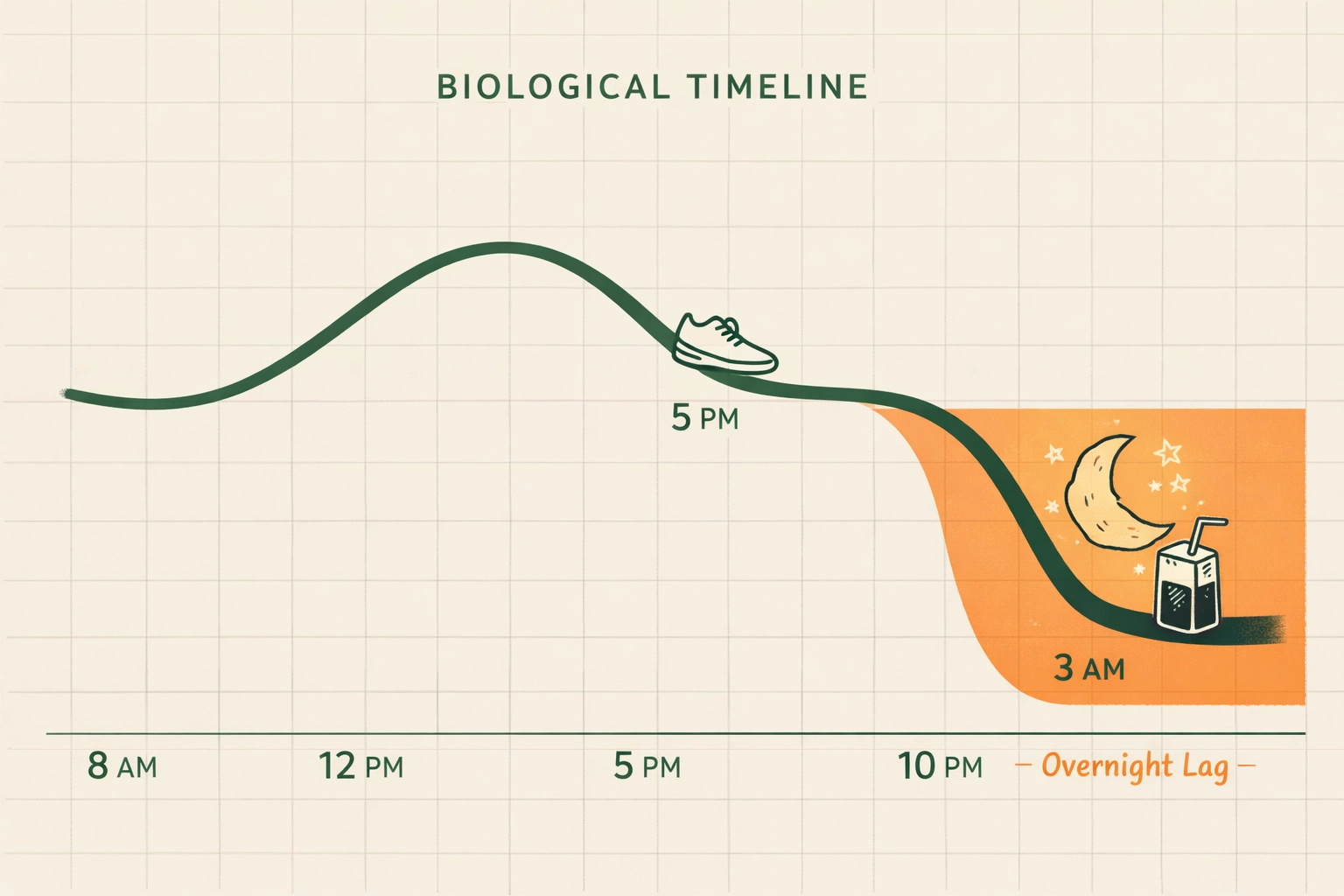
We’ve all been there. You finish your workout, you bolus for the high (or eat for the low), and you feel stable. Then, 8 hours later, usually at 3 AM, your CGM alarm starts screaming.
This is the "Lag Effect," or what some call the "Sore Muscle Low."
When you exercise hard, you deplete the glucose stored in your muscles (glycogen). Once you stop, your body spends the next several hours trying to "refill the tank." It pulls glucose from your blood to replenish those stores.
This process increases your insulin sensitivity for up to 24 hours. If you don't account for this by lowering your basal rate or having a protein-heavy snack before bed, you’re on a collision course with a midnight juice box. It’s not a failure of your management; it’s just your biology doing its job.
It feels counterintuitive to give yourself insulin before working out, especially when we’re so afraid of lows. But if you’re doing high-intensity (anaerobic) work, you might actually need a "correction" or a different basal strategy.
This is where the "Veteran" experience kicks in. We know that the gym doesn't exist in a vacuum.
We’re told to just "test more" or "eat more sugar," but that’s a reactive way to live. It keeps us in a state of constant anxiety.
The goal isn't to perfectly predict every single 3-mile run. The goal is to build a "library" of how your body reacts.
Maybe you realize that "Heavy Leg Day" always spikes you by 50 points, but "Chest Day" keeps you flat. Maybe you notice that if you run after 6 PM, you always go low at 2 AM, but morning runs don't have that effect.
This is exactly why we built Subseven. We were tired of the "invisible load", the mental gymnastics of trying to remember how last Tuesday’s run went while staring at a plummeting CGM line.
By logging these hidden variables, the intensity, the sleep, the stress, you stop being a victim of the chaos. You start seeing the "Why" behind the "WTF." When you understand the pattern, you regain the freedom to push your body without the fear of the crash.
Exercise is worth the trouble. The mental clarity, the heart health, the improved sensitivity, it’s all real. You just need a system that’s as smart as the challenges T1D throws at you.
Q: Should I exercise if my blood sugar is over 250?
A: Check for ketones first. If ketones are present, avoid exercise, as it can actually push you toward DKA. If ketones are negative, a light walk might help, but be cautious with high-intensity workouts which could spike you higher.
Q: Why does my blood sugar drop during a walk but rise during a sprint?
A: Walking is aerobic (uses blood glucose for fuel), while sprinting is anaerobic (triggers adrenaline, causing the liver to dump stored glucose).
Q: How long does the "exercise effect" last on insulin sensitivity?
A: You can experience increased insulin sensitivity for 12 to 24 hours after a workout as your body works to replenish muscle glycogen.
Q: Is it better for T1Ds to exercise in the morning or evening?
A: There is no "better" time, but many find morning exercise more predictable because they have less "Insulin on Board" from meals and a higher natural cortisol level to prevent lows.
Q: How can I prevent the 3 AM crash after a workout?
A: Try reducing your basal rate by 10-20% overnight after a hard workout, or have a snack containing protein and fat before bed to provide a steady energy source.
Q: Does fitness level affect blood sugar spikes?
A: Yes. As you get fitter, your body becomes more efficient at using fuel and your hormonal "stress" response to the same level of exercise often decreases, leading to more stable numbers.
Author Bio:
Chris Putsch is the CEO of Subseven and has lived with Type 1 Diabetes for over 20 years. He’s an avid athlete who spent years fighting the "exercise rollercoaster" before building the tools he wished he had at diagnosis. He's on a mission to take the stressing and guessing out of T1D management.